|
A Blended Approach to Emergency Medicine Training: Developing an Integrated Curriculum for Mature Learners Ian Sammy, Dept of Clinical Surgical Sciences Abstract
INTRODUCTION In January 2005, the REVIEW OF THE LITERATURE Traditionally, emergency rooms have
been managed by junior doctors from a variety of specialties, with a variable
degree of advice and support from their senior colleagues, usually over the
telephone. In the early 1970’s this approach was recognised as inefficient at
best, as patients often had to go through a series of repetitive examinations
by increasingly senior staff before any effective clinical decisions were
made. Furthermore, the system could be
dangerous and even life-threatening to seriously ill or injured patients. These
patients often need resuscitative care immediately, and delays in providing
such care could be costly in terms of patient morbidity and mortality. In light
of these findings, the specialty of Emergency Medicine was developed. These doctors provide immediate
emergency and resuscitative care to all patients presenting to Emergency
Departments with acute problems. Introducing Emergency Medicine training and
the provision of trained Emergency Physicians for the management of patients
has improved outcomes for critically ill patients (Melniker & Leo 1998;
Wyatt, Henry et al. 1999; Lecky, Woodford et al. 2000). It is also evident that
direct supervision of junior doctors has improved the care of individual
patients and allowed the more efficient use of resources (Sacchetti, Carraccio
et al. 1992; Cooke, Kelly et al. 1998).
As a result, patients are less likely to be unnecessarily admitted to
hospital, inappropriately discharged or sent for needless investigations if
seen by a trained Emergency Physician. Moreover, outcomes for patients with
multiple trauma and acute cardiac conditions have improved with the better
organization of Emergency Departments and resuscitation teams (Cales 1984; Mann
& Heyworth 1996). In light of the above, it has been recognised that
Emergency Medicine is an essential aspect of acute medical care, and specific
training in this specialty would improve outcome in our most seriously ill and
injured patients. Emergency Medicine is a relatively
new specialty throughout the world. Training today’s clinicians to manage
emergency and disaster medicine requires effective, flexible, just-in-time
learning. Blended learning is playing an increasing role in medical education
and its strategies include combining traditional classroom activities with
multimedia materials (e.g. video clips), online discussions and computer based
assessment (Davies, Ramsay et al. 2005). By combining e-learning technologies
with traditional instructor-led training, a shift from the passive
teacher-centred model of education to an active learner-centred model is
occurring (Ruiz, Mintzer et al. 2006). Today’s e-learning programmes go beyond
delivering information to encourage independent learning and include
communication and information handling, clinical skills, patient investigation
and management, decision making and ethics (Harden 2002). Blended approaches to clinical
training have been successfully applied in emergency and disaster medicine
achieving significant improvements in knowledge, clinical and communication
skills (Della Corte, La Mura et al. 2005; Gordon, Issenberg et al. 2005; Miller,
Scott et al. 2006). Blended learning models may comprise different concepts
including combining different modes of delivery, different instructional
strategies and/or different technologies (Driscoll 2002). E-learning activities
involve computers and interactive networks (Tsai & Machado 2002).
E-learning will not replace teachers but it will change the roles of the
teacher and student: teachers will become designers of learning experiences and
students will be connected to others as they collaborate and take on the role
of the teacher. No matter the model used, the mix of instructor-led and
self-directed learning; synchronous and asynchronous interaction with peers,
instructor and content; and supplementing learning with practice; provides
choice, promotes engagement and improves performance. This multi-modal,
multimedia way of teaching is about getting the “right content in the right
format to the right people at the right time” (Singh 2003). While blended learning has been used
to good effect in Emergency Medicine for some years now, most specialist
programmes have concentrated on full time residency programmes, such as the
Fellowship of the College of Emergency Medicine (FCEM) training in the United
Kingdom, the Fellowship of the Australasian College for Emergency Medicine
(FACEM) in Australia and various residency programmes in the United States (Leman
1997; Wyatt & Weber 1998). This effectively excludes many potential
candidates from specialist training, including practitioners working in
isolated or rural areas, not able to return to full time training, and primary
care doctors who wish to increase their knowledge and practice of Emergency
Medicine, but do not require full specialist training or qualification. Only
the Canadian system of training allows for a shortened period of training in
Emergency Medicine for those doctors who have already trained in Family
Medicine, but wish to further specialise in Emergency Medicine (one year as
opposed to the traditional four year residency for those coming straight out of
internship). We know of no other programme which offers part time training to
doctors who are unable to avail themselves of a full time residency programme. Such a programme is of particular
importance in areas such as the MATERIALS AND METHODS This is an observational analysis of
the first year of the MSc course. The paper describes the teaching methods used
throughout the course, and maps the methods and assessment strategies to the
educational objectives, while discussing their appropriateness. Approximately
six (6) months after the end of the first year of the course, focus group
discussions were conducted with the entire group of participants. During the 90 minute session, evaluation
questions were posed on: the educational experience; relevance of materials
presented; scope of information presented and applicability to current
practice. RESULTS The programme has used a variety of
educational tools and approaches in achieving its objectives. These have been
chosen to best suit the material presented, and different educational styles
have been combined in specific areas of the course to reinforce the main
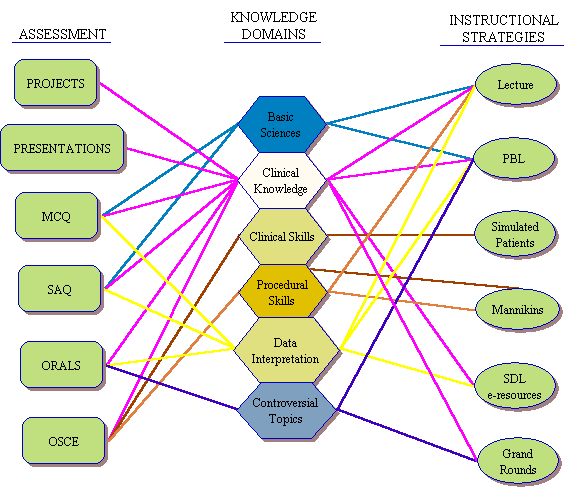
learning objectives of these topics. Figure 1 maps the knowledge domains
against both the instructional methods and assessment strategies used in the
programme. All modules in the first year were clinically based, and as such the
learning methods were chosen to reflect the need for clinical knowledge, as
well as clinical and procedural practice, where appropriate. Furthermore, certain
clinical data interpretation skills were enhanced by the use of self-directed,
computer based tools. This was particularly useful in the case of
interpretation of x-rays, ECGs and laboratory tests. Resuscitation skills, in particular,
were enhanced by the use of internationally recognised short courses, which
were mandatory for all candidates. These included courses in cardiac and
paediatric resuscitation, and emergency airway management (all critical areas
of management in Emergency Medicine). While these courses were evaluated very
positively by candidates, it was felt that some direct clinical teaching or
supervision would have helped consolidate the lessons learned in the courses.
Skills learned on these courses were also supplemented by less formal skills
training sessions throughout the year. The resuscitation courses described
above are used internationally to train doctors and other health care
professionals in these essential skills. Interestingly, it is generally
recognised that skill retention is less in participants who do not use them
regularly in the workplace (Mancini & Kaye 1985; Carley & Driscoll
2001). This reinforces our candidates’ view that the skills require
consolidation with clinical supervision in the workplace. Communication skills were taught
using simulated patients, and peer practice (candidates playing the part of
patients). Both these methods were viewed positively by candidates, who saw the
need for and benefit of these sessions. Communication skills are now seen as an
essential part of good medical practice by the General Medical Council (GMC) of
the On the whole, candidates’ reactions
to the course were positive. While in most cases it was clearly a challenge for
them to return to the classroom after many years and they needed to adjust to
new methods of learning, there was support for this transition. In particular,
the Medical Sciences Library was a valuable resource offering an orientation to
the use of information technology and a portal for gaining access to
information. Other adjustments included the need for structured reading and
study, using information technology, practising with simulated patients and
taking part in skills training. Candidates indicated a high degree of
satisfaction with the course material. They felt that the material was both
relevant and applicable to their practice. Specifically, materials presented in
electronic format and intended for independent learning were used readily by
candidates. Benefits of the programme (in the
eyes of the candidates) were surprisingly diverse. Candidates felt that the
course brought them up to date with international standards in the specialty,
and brought focus and clarity to an area of medicine which was hitherto
perceived as vague and ill-defined. They appreciated Emergency Medicine as a
specialty in its own right, with its own priorities and treatment protocols, as
opposed to it being a subordinate of other more well-recognised specialities
(such as surgery or internal medicine). Furthermore, they were able to evaluate
critically their own practice through a process of audit. At least one
candidate explained that he identified weaknesses in clinical practice in his
department, and was able to implement meaningful change by this process.
Additionally, candidates felt that they were able to reflect positively on the
specific learning needs which emerged during the course of the year, and respond
positively to these. Interestingly, most candidates recognised an
administrative advantage to the learning experience, as they were better able
to identify resource and management needs within their departments, and
successfully lobby for change. Some of these needs included the acquisition of
new equipment, the education of other members of staff and the promotion of new
and more effective ways of practicing clinical medicine in the emergency
setting. At least one of the candidates admitted that his role was more of an
administrative one, but that he had been able to make better decisions
regarding his department because of this course. Most of the candidates saw
themselves as agents for change (rather than just better clinicians) after
having attended the course. With regard to possible areas for
improvement, candidates felt that the end of year examination was a particular
challenge to them, and that more specific examination preparation would have
been useful. Having said this, they identified certain areas of the examination
which were particularly well designed and relevant. The computer-based data
interpretation examination was singled out as an example of a good assessment
tool. It appears that not all the examiners were as comfortable with the assessment
methodologies as was required. Candidates particularly had difficulties with
some of the clinical examination stations (OSCE), and parts of the oral
examination station. However, they felt sufficiently confident in their
knowledge to challenge the assertions of examiners when they thought that the
examiners’ interpretations of the clinical scenarios were incorrect. In
addition, they felt that the external examiner was quite impressed with their
overall performance, and this certainly enhanced their self-confidence.
Candidates were pleased with both the content and delivery of the course, and
felt that it should be accessible to a wider audience of participants, as this
would help to influence the development of Emergency Medicine in the country,
and support much needed change in this field of medicine. DISCUSSION The MSc in Emergency Medicine of the
University of the West Indies, Cales, R. H. (1984), "Trauma
mortality in Carley, S. & Driscoll, P.
(2001), "Trauma education", Resuscitation,
vol. 48, no. 1, pp. 47-56. Cooke, M. W., Kelly, C., Khattab,
A., Lendrum, K., Morrell, R. & Rubython, E. J. (1998), "Accident and
emergency 24 hour senior cover--a necessity or a luxury?" Journal of Accident and Emergency Medicine, vol.
15, no. 3, pp. 181-184. Davies, A., Ramsay, J., Lindfield,
H. & Couperthwaite, J. (2005), "A blended approach to learning: added
value and lessons learnt from students’ use of computer-based materials for
neurological analysis", British
Journal of Educational Technology, vol. 36, no. 5, pp. 839-849. Della Corte, F., La Mura, F. &
Petrino, R. (2005), "E-learning as educational tool in emergency and
disaster medicine teaching", Minerva
Anestesiologica, vol. 71, no. 5, pp. 181-195. Driscoll, M. (2002), "Blended
learning", e-learning, vol. 3,
no. 3, pp. 54. Gordon, D. L., Issenberg, B.,
Gordon, M. S., LaCombe, D., McGaghie, W. C. & Petrusa, E. R. (2005),
"Stroke training of prehospital providers: an example of
simulation-enhanced blended learning and evaluation", Medical Teacher, vol. 27, no. 2, pp. 114-121. Harden, R. M. (2002), "Myths
and e-learning", Medical Teacher, vol.
24, no. 5, pp. 469-472. Lecky, F., Woodford, M. & Yates,
D. W. (2000), "Trends in trauma care in England and Wales 1989-97", Lancet, vol. 355, no. 9217, pp.
1771-1775. Leman, P. (1997), "Emergency
medicine training in Mancini, M. E. & Kaye, W.
(1985), "The effect of time since training on house officers' retention of
cardiopulmonary resuscitation skills." The
American Journal of Emergency Medicine, vol. 3, no. 1, pp. 31-32. Mann, C. J. & Heyworth, J.
(1996), "Comparison of cardiopulmonary resuscitation techniques using
video camera recordings." Journal of
Accident and Emergency Medicine, vol. 13, no. 3, pp. 198-199. Melniker, L. A. & Leo, P. J.
(1998), "Comparative knowledge and practice of emergency physicians,
cardiologists, and primary care practitioners regarding drug therapy for acute
myocardial infarction", Chest, vol.
113, no. 2, pp. 297-305. Miller, G. T., Scott, J. A.,
Issenberg, S. B., Petrusa, E. R., Brotons, A. A., Gordon, D. L., McGaghie, W.
C. & Gordon, M. S. (2006), "Development, implementation and outcomes
of a training program for responders to acts of terrorism", Prehospital Emergency Care, vol. 10, no.
2, pp. 239-246. Ruiz, J. G., Mintzer, M. J. & Sacchetti, A., Carraccio, C. &
Harris, R. H. (1992), "Resident management of emergency department
patients: is closer attending supervision needed?" Annals of Emergency Medicine, vol. 21, no. 6, pp. 749-752. Singh, H. (2003), "Building
effective blended learning programs", Educational
Technology, vol. 43, no. 6, pp. 51-54. Tsai, S. & Machado, P. (2002),
"E-learning, online learning, web-based learning, or distance learning:
unveiling the ambiguity in current terminology", eLearn, vol. 2002, no. 7, pp. 3. Wyatt, J. P., Henry, J. & Beard,
D. (1999), "The association between seniority of Accident and Emergency
doctor and outcome following trauma", Injury,
vol. 30, no. 3, pp. 165-168. Wyatt, J. P. & Weber, J. E.
(1998), "A transatlantic comparison of training in emergency
medicine", Journal of Accident and
Emergency Medicine, vol. 15, no. 3, pp. 175-180. Figures |